Medical Billing Services Company
Save 25% More Revenue with Our AI-Powered Medical Billing Services


Claims Managed
Growth Impact
Up to 35% Denial Reduction
Error-Free coding, payer checks, and faster denial follow-up.

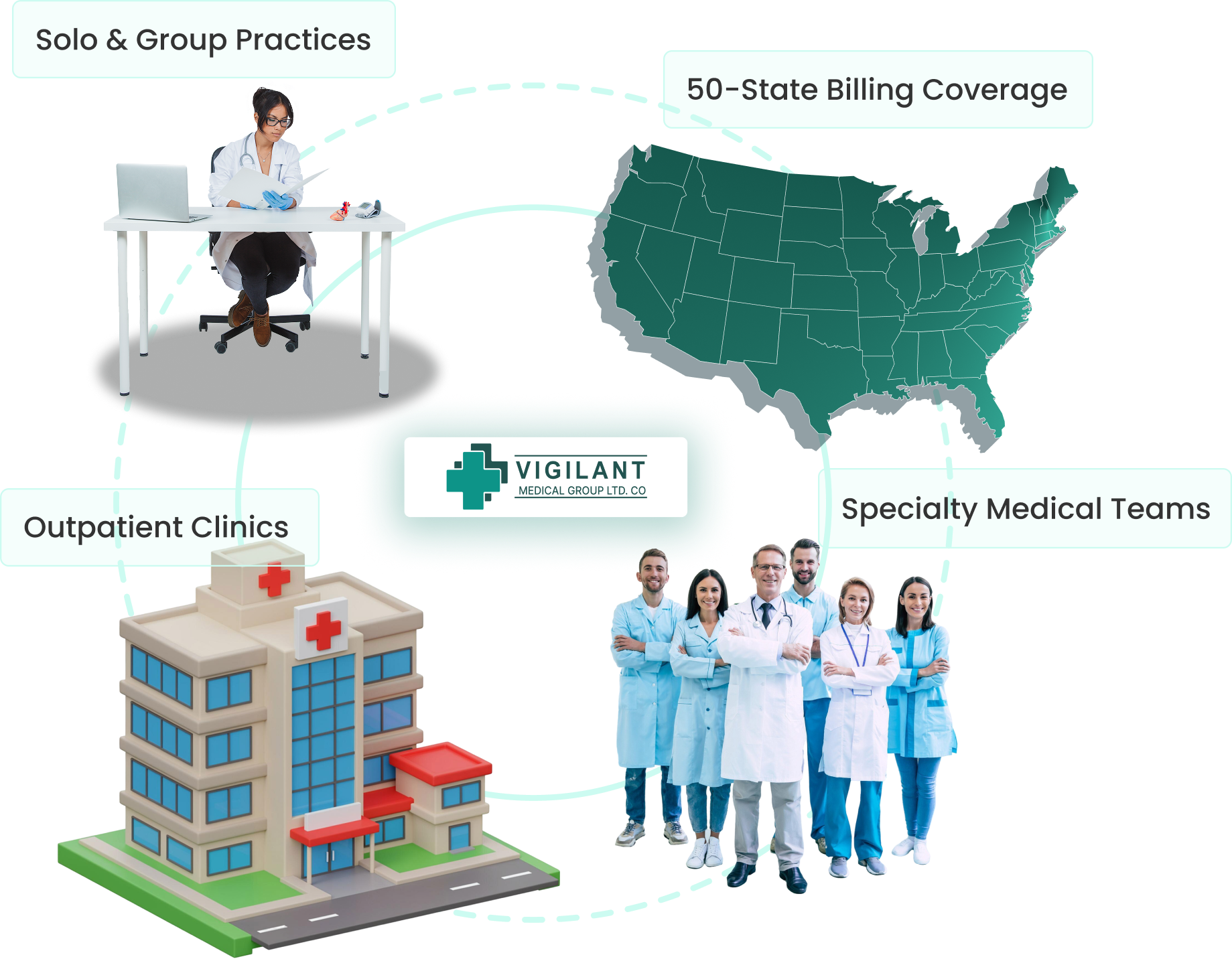
Medical Billing Services Provider Offering 99.4% Clean Claims & Smoother Revenue Cycles
Every denied claim, delayed payment, and missed follow-up puts revenue at risk. With claim denial rates reaching nearly 12% and providers spending billions each year fighting payer pushback, even small RCM gaps can become costly. Vigilant Medical Group helps practices stop revenue from being lost through the small gaps, so providers can stay focused on patient care while the financial side stays under control.
With 500+ specialty-trained certified expert billers and coders, our medical billing company delivers 99.4% clean claims, faster follow-ups, smarter denial handling, and accurate reimbursements.
Hiring a general billing team that does not understand your specialty can lead to coding mistakes, denied claims, delayed payments, and compliance risks.
Work with specialty-trained medical billing experts who understand payer rules, clean claim submission, denial prevention, and accurate reimbursement for your practice.
All-In-One AI-Powered Medical Billing Services
Vigilant Medical Group stands among the best medical billing companies in Texas and all 50 states. We offer flexible clinical billing services for medical practices that need cleaner claims, stronger follow-up, and better revenue visibility.

Medical Billing
We submit clean claims, review EOBs/ERAs, post payments, manage denials, and keep reimbursements moving.
Provider Credentialing
Our credentialing specialists enroll providers with payers, manage credential updates, and help prevent contract and approval delays.
Healthcare RCM
As an MSO company, we manage the full revenue cycle, lower AR days, improve collections, and support steady cash flow.
Medical Coding
Our certified coders handle ICD-10, CPT, and HCPCS coding with accuracy, stronger documentation, and lower audit risk.

Our Billing Agency Beats All Challenges
Practices lose 10%–12% of net revenue annually due to denials and coding errors
Vigilant Medical Group Has a Solution!
- Medical Coding Errors
- Missing ICD-10 details (laterality, acuity) trigger denials.
- Wrong CPT/modifier use causes bundling or duplicate denials.
- Weak documentation fails medical necessity and increases audit risk.
- Prior Auth & Medical Necessity
- Approved authorizations still deny when claim details don’t match.
- Missing clinical notes trigger medical necessity denials and repeat requests.
- Each review cycle can add 45–60 days to the payment timeline.
- ERA Posting & Payment Variance
- Wrong CARC group mapping shifts balances and write-offs incorrectly.
- Underpayments hide in adjustments without contract-rate checks.
- Slow follow-up risks timely filing and appeal deadlines.


- Accurate Medical Coding Support
- We review ICD-10 details before claims go out.
- CPT and modifier checks help reduce avoidable denials.
- Documentation gaps are flagged before they become audit issues.
- Prior Auth & Necessity Review
- We match claim details with approved authorizations.
- Clinical notes are checked before payer submission.
- Faster follow-up helps reduce long review delays.
- ERA Posting & Payment Checks
- CARC/RARC codes are reviewed for accurate posting.
- Contract rates are checked to catch underpayments.
- Follow-ups are tracked before appeal deadlines are missed.
Learn How Vigilant Medical Group Can Make a Difference
What Healthcare Providers Say About Our Medical Billing Services

31%
Average Reduction in Denials for Clients
“We were losing payments on Texas Medicaid and MCO claims because authorizations, diagnosis details, and clinical notes were not lining up the way payers required. Vigilant reviewed each claim against Texas payer rules, matched the authorization to the billed service, corrected documentation gaps, and resubmitted with stronger support. Their medical billing Texas helped us reduce repeat denials and get payments moving faster.”
Dr. Daniel Collins
Owner, Northpoint Orthopedic Clinic, Texas
Dr. Rachel Morgan
Medical Director, Lakeside Family Care
Dr. Melissa Grant
Practice Lead, Westbrook Internal Medicine
“We were missing underpayments because adjustments were posted without checking payer contracts. Vigilant reviewed our ERA posting, CARC/RARC codes, and contracted rates. They found payment variances we were overlooking and helped us recover revenue that would have stayed hidden.”
Dr. Jason Reed
Administrator, Clearview Surgical Group
Want to Recover 20% More Revenue this Year?
Let our team handle the billing complexity so your practice can stay focused on patient care.
- HIPAA-conscious workflows
- Built for practices, groups, & specialty billing
KPI-Led Billing Services for Faster Payments & Growth
95-99.4%
First Pass Claim Rate
Denial Rate
Under 3%
Up to 25%
Net Revenue Growth
Recover underpayments, prevent write-offs, and catch missed charges weekly.
Payment Posting
within
Under 24-48 Hours
Post ERAs fast, reconcile EOBs, and map adjustments correctly to keep A/R clean.
A/R Days Under 38
95–98%
Coding Accuracy
Compliance Expertise Built Into Every Step of Your Medical Billing Services
Compliance issues often happen when payer rules are missed, documentation is weak, or patient data is handled without proper controls. These mistakes can lead to denied claims, audits, repayment demands, and HIPAA penalties that may reach thousands of dollars per violation. Our compliance-focused RCM team reviews coding, claims, documentation, posting, and follow-up to keep your billing accurate, secure, and audit-ready.
Payer Compliance
CMS & Insurance Rules
Core Focus Areas
- Coverage checks
- Claim edits
- LCD/NCD review
- Payer rule updates
HIPAA Compliance
Protected Billing Workflows
Core Focus Areas
- PHI security
- Limited access
- Safe data use
- Workflow controls
State Law Compliance
Rules That Vary by State
Core Focus Areas
- State billing laws
- Patient notices
- Payment rules
- Practice oversight
A Smarter Medical Billing Process Made to Protect Every Payment

Eligibility & Patient Verification
We confirm patient details, insurance coverage, and plan benefits before the visit. If prior authorization is needed, our team checks the requirements early so claims do not get delayed later.
- Fewer eligibility denials.
- Clear patient cost share.
- Fewer claim surprises.

Accurate Coding Review
Our CPB-certified coders review diagnosis codes, procedure codes, modifiers, and documentation before claims are sent. This helps reduce coding errors and improves first-pass claim acceptance.
- Fewer coding denials.
- Cleaner claims.
- Lower audit risk.

Clean Claim Submission
We check each claim for missing details, payer rules, provider information, and claim errors before submission. Rejections are tracked quickly, corrected, and resubmitted without delay.
- Fewer payer rejections.
- Faster claim acceptance.
- Better payment flow.

Denial Follow-Up
We sort denied claims by reason, review what caused the issue, and take the right action. Claims are corrected, appealed, and followed until the payer gives a final response.
- Faster recovery.
- Less aging AR.
- Stronger appeal results.

Payment Posting & Patient Billing
We post payments, adjustments, and patient balances accurately. After insurance processing, we send clear patient statements and help reduce confusion around what is owed.
- Accurate balances.
- Fewer billing disputes.
- Smoother collections.
Our Certifications
We maintain industry-recognized certifications that reflect our commitment to data security, compliance, and operational integrity. Our workflows are built around HIPAA compliance standards and ISO 27001-certified information security practices, ensuring that your patient data, billing information, and financial records are handled with strict protection and control.

State Compliant Medical Billing Company Serving All 50 States
Our medical billing experts understand that every state has different payer rules, so we manage workers’ comp, Medicaid, and compliance changes across all 50 states.
- Medical billing company headquartered in Texas
- RCM support built for practices of every size
- State law and billing laws experts

Specialized Texas-Based Support for Smarter Medical Billing
As the best medical billing company in Texas, Vigilant Medical Group understands how Texas payer rules can slow down clean reimbursements. That’s why our medical billing services in Texas are specially built around TDI clean-claim standards, Medicaid/TMHP requirements, MCO authorization rules, payer edits, and contract-based payment checks.
- Texas Prompt Pay timelines tracked before claims age
- TMHP and Medicaid claim rules reviewed before submission
- MCO authorizations matched with service and diagnosis details
- Contract rates checked to catch underpaid Texas claims
Want to Recover 20% More Revenue this Year?
Let our team handle the billing complexity so your practice can stay focused on patient care.
- HIPAA-conscious workflows
- Built for practices, groups, & specialty billing
Specialty-Based Healthcare Billing Company
Medical billing becomes more complex with specialty-specific coding, documentation, and payer rules. Since each specialty has different requirements, so our medical billing agency assigns specialty-based experienced billers and coders to ensure accurate, compliant claims.
Payer Work That Goes Beyond Basic Claim Submission
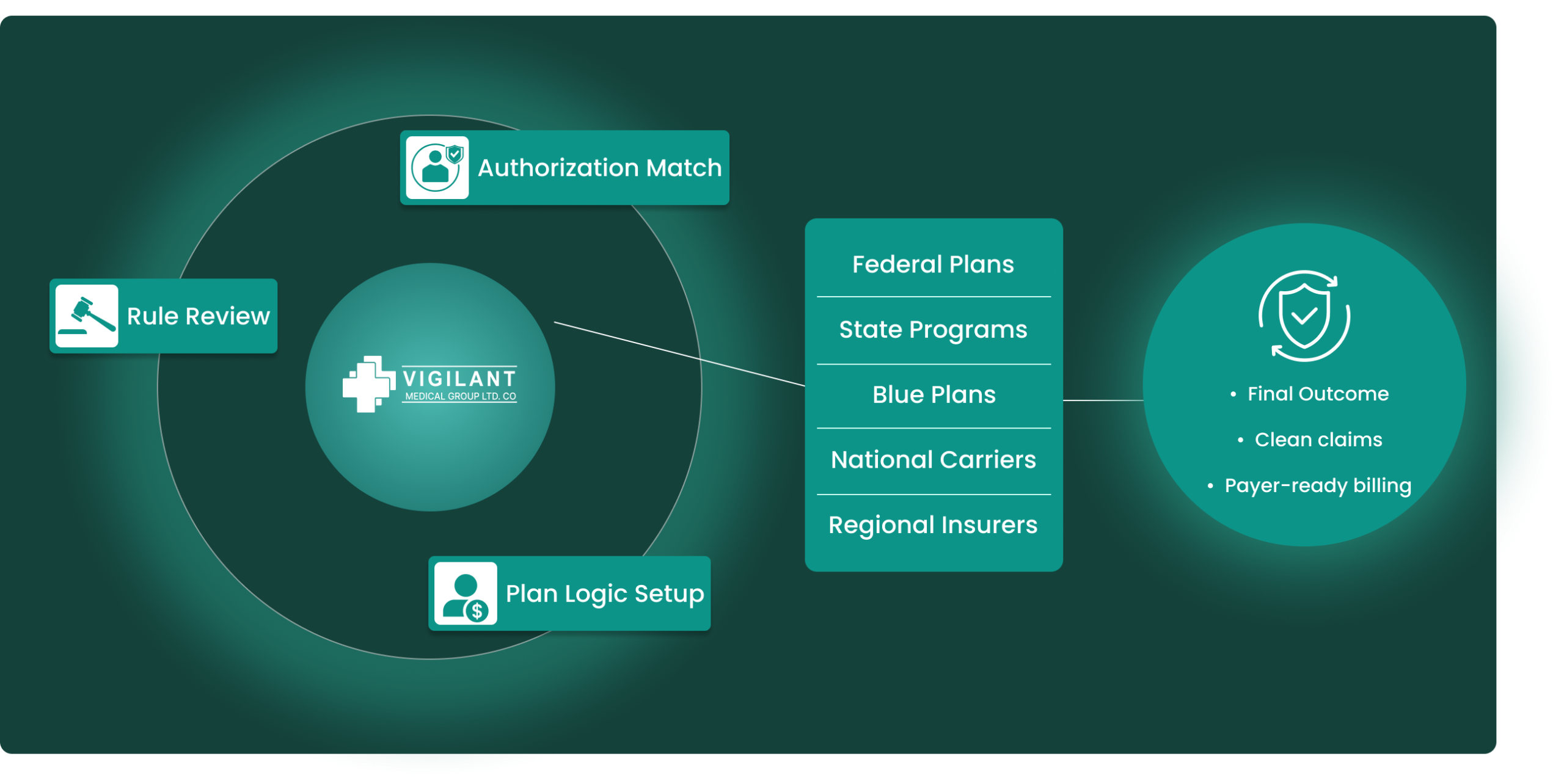
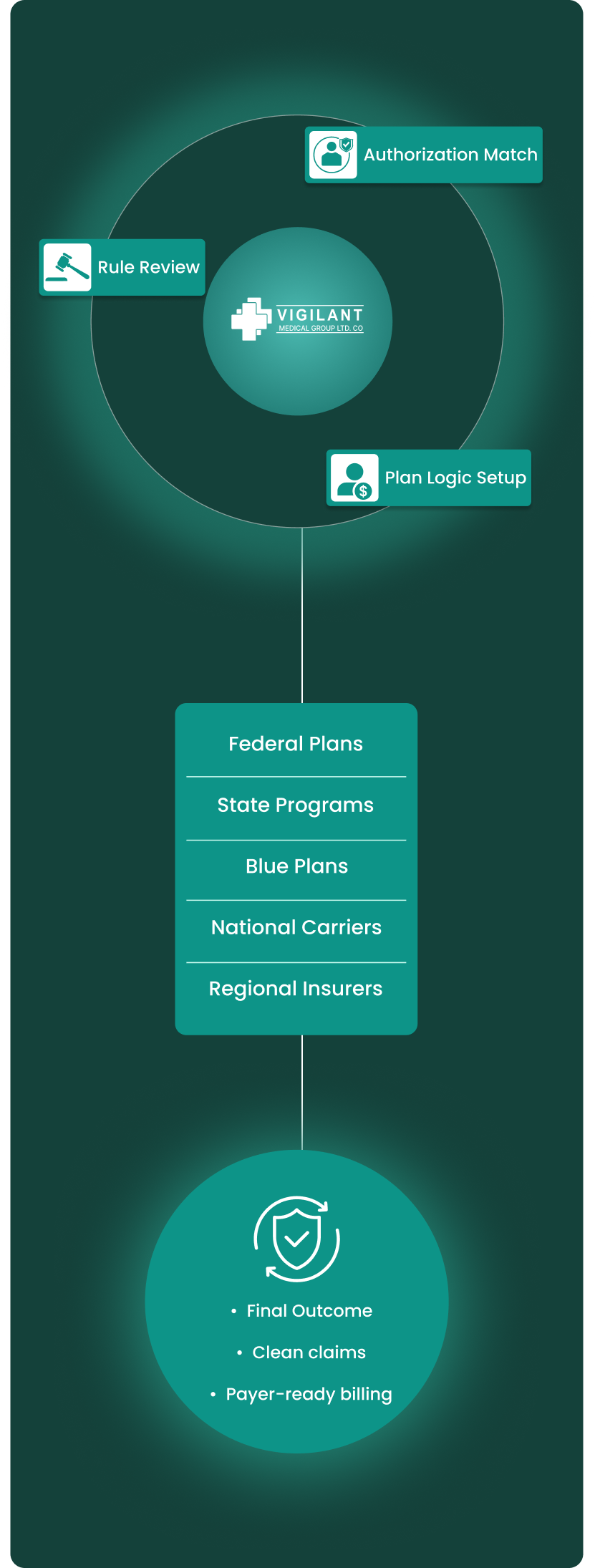
Medicare
We check Medicare claims against visit notes, diagnosis support, modifiers, and coverage limits before submission. When a denial happens, we review the reason, correct the issue, and prepare the claim or appeal with the right documentation.
Medicaid
Medicaid billing needs state-level accuracy and plan-specific handling. We manage traditional Medicaid, Medicaid Advantage, Managed Care, and MCO claims to reduce delays and protect payment accuracy.
Commercial Payers
Commercial plans often deny or underpay based on contract terms, prior auth rules, COB, and plan-specific edits. We compare claim details with payer requirements, flag underpayments, and follow up until the balance is addressed.
Workers' Compensation
Workers' Comp claims require careful handling because payment depends on injury details, employer coverage, adjuster communication, authorization status, and state-specific billing rules. We help practices manage these claims with accuracy so that valid services do not remain unpaid or delayed.
Personal Injury / Liens
Personal injury and lien-based cases need strong coordination between providers, attorneys, patients, and payers. We help track treatment-related balances, maintain lien accuracy, support documentation needs, and keep accounts organized until settlement or payment resolution.
Which billing problems are costing your practice the most right now?


Your EHR & EMR Stays the Same With Us
Vigilant Medical Group works inside your existing system, reviews claim data at the source, updates billing activity, and keeps your RCM workflow moving without forcing your team to change platforms.
Customized Medical Billing Services for Your Practice
Vigilant Medical Group provides services to practices of all types and sizes, including solo providers, group practices, hospitals, and multi-location clinics. Our medical billing company in Texas adjusts our billing workflow to match your volume, payer mix, and specialty needs. When you outsource medical billing to companies in USA we are known as one of the best for providing affordable and flexible billing solutions across all US states.
Anesthesia billing services
We handle anesthesia billing with accurate time units, modifiers, ASA codes, payer rules, and follow-up to reduce denials and protect payments.
Medical Billing for Small Practices
We provide right-sized billing support for smaller teams that need strong controls without extra overhead.
Hospital Billing Services
Vigilant Billing offers high-volume hospital billing services with audit-ready compliance, coding, posting, and denial management.
Physician Billing Services
Our experts support practices by managing claims, timely filing, underpayments, and balances for faster payments.
Medical Billing Cost Saver Guide
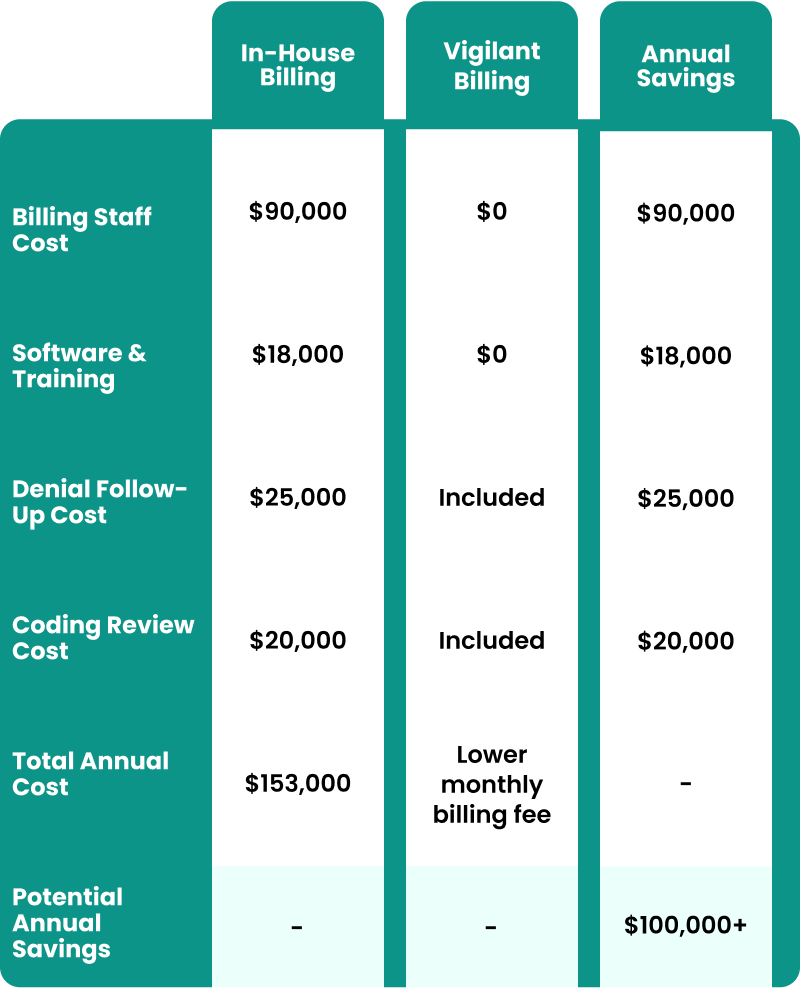
In-House Billing
Vigilant Billing
Annual Savings
Billing Staff Cost
$90,000
$0
$90,000
Software & Training
$18,000
$0
$18,000
Denial Follow-Up Cost
$25,000
Included
$25,000
Coding Review Cost
$20,000
Included
$20,000
Total Annual Cost
$153,000
Lower monthly billing fee
-
Potential Annual Savings
-
-
$100,000+
Get Instant FREE Pricing Quote
$50k
Collections
Dr. Jessica Humphrey
Frequently Asked
Questions
Trusted in 50 States by 500+ Providers
Medical Billing Services
What type of medical billing services do you offer?
Our medical billing company USA provides full claims billing service support from eligibility checks to charge entry, claim submission, denial follow-up, and payment posting. Each healthcare provider or practice also gets dedicated Account Managers for updates and questions.
Do you work with major payers like Blue Cross Blue Shield?
Yes, our expert medical billers work with Blue Cross Blue Shield and many other commercial and government payers across USA Healthcare. We follow payer-specific rules so claims move faster and denials drop.
Do you provide medical billing services in Texas?
Yes, when you outsource billing services, our medical billing firm hires billing teams who specialize in rules, documentation, and payer edits across 50+ specialties. This improves coding accuracy and helps medical practices avoid repeat denials.
Does Vigilant Medical Group provide provider credentialing services?
Yes, our credentialing specialists manage enrollments, recredentialing, and payer updates. This keeps the healthcare provider active with payers and prevents claim delays caused by enrollment issues.
Pricing
How do you price your medical billing services?
Pricing for our medical billing services USA depends on your volume, specialty, and workflow needs. As a healthcare billing services company, we offer plans that can be percentage-based, flat monthly, or hybrid.
What is included in the monthly fee?
Most plans include claims processing, denial follow-up, posting, reporting, and Account Managers’ support.
Are there any setup fees?
Some projects have a one-time setup for intake, EHR access, payer connectivity, and workflow mapping. Your billing service provider will confirm this upfront, so there are no surprises.
Can pricing change as we grow?
Yes, we adjust pricing when claim volume or service scope changes. This keeps your billing firm aligned with your growth and keeps service levels consistent.
EHR
Do you work with my EHR?
Yes. Our medical billing service providers can work inside your EHR or through secure access, depending on your practice setup and permissions.
Will I need to switch systems or my EHR?
No, most healthcare providers keep their current EHR. Our medical billing services company fits into your workflow so Physicians and staff do not face disruption.
How do you get charges and notes for coding?
We use your EHR data and your documentation flow to support coders and billing teams. If your process includes medical transcription, we can align transcription outputs with coding and charge capture.
How long does EHR onboarding take?
It depends on access, data quality, and payer setup. Your Account Managers will share a clear onboarding plan and keep you updated at each step.
Compliance
How do you keep billing compliant?
We follow HIPAA policies, payer billing rules, state laws, and coding guidelines. Our medical billing firm also uses quality checks so claims match documentation and reduce audit risk.
Do you support coding compliance?
Yes, our certified coders review ICD codes, CPT coding, and modifiers based on payer rules and specialty documentation for claim accuracy and compliance.
How do you handle documentation gaps?
We flag missing details early and share clear feedback with the healthcare provider. This helps Physicians improve documentation so claims are supported and compliant.
Who oversees compliance on your side?
Our billing teams include experienced leaders and trained staff, including CPB and RHIA credentialed professionals where required. This adds strong oversight for accuracy, privacy, and process control.
What type of medical billing services do you offer?
Our medical billing company USA provides full claims billing service support from eligibility checks to charge entry, claim submission, denial follow-up, and payment posting. Each healthcare provider or practice also gets dedicated Account Managers for updates and questions.
Do you work with major payers like Blue Cross Blue Shield?
Yes, our expert medical billers work with Blue Cross Blue Shield and many other commercial and government payers across USA Healthcare. We follow payer-specific rules so claims move faster and denials drop.
Do you provide medical billing services in Texas?
Does Vigilant Medical Group provide provider credentialing services?
Yes, our credentialing specialists manage enrollments, recredentialing, and payer updates. This keeps the healthcare provider active with payers and prevents claim delays caused by enrollment issues.
How do you price your medical billing services?
Pricing for our medical billing services USA depends on your volume, specialty, and workflow needs. As a healthcare billing services company, we offer plans that can be percentage-based, flat monthly, or hybrid.
What is included in the monthly fee?
Most plans include claims processing, denial follow-up, posting, reporting, and Account Managers’ support.
Are there any setup fees?
Some projects have a one-time setup for intake, EHR access, payer connectivity, and workflow mapping. Your billing service provider will confirm this upfront, so there are no surprises.
Can pricing change as we grow?
Yes, we adjust pricing when claim volume or service scope changes. This keeps your billing firm aligned with your growth and keeps service levels consistent.
Do you work with my EHR?
Yes. Our medical billing service providers can work inside your EHR or through secure access, depending on your practice setup and permissions.
Will I need to switch systems or my EHR?
No, most healthcare providers keep their current EHR. Our medical billing services company fits into your workflow so Physicians and staff do not face disruption.
How do you get charges and notes for coding?
We use your EHR data and your documentation flow to support coders and billing teams. If your process includes medical transcription, we can align transcription outputs with coding and charge capture.
How long does EHR onboarding take?
It depends on access, data quality, and payer setup. Your Account Managers will share a clear onboarding plan and keep you updated at each step.
How do you keep billing compliant?
We follow HIPAA policies, payer billing rules, state laws, and coding guidelines. Our medical billing firm also uses quality checks so claims match documentation and reduce audit risk.
Do you support coding compliance?
Yes, our certified coders review ICD codes, CPT coding, and modifiers based on payer rules and specialty documentation for claim accuracy and compliance.
How do you handle documentation gaps?
We flag missing details early and share clear feedback with the healthcare provider. This helps Physicians improve documentation so claims are supported and compliant.
Who oversees compliance on your side?
Our billing teams include experienced leaders and trained staff, including CPB and RHIA credentialed professionals where required. This adds strong oversight for accuracy, privacy, and process control.
Map Directions
Building 1809 Possum Fire Trail, Mesquite TX 75181
Let's Talk
Primary: +1-469-799-5556
Secondary +1-945-994-8898
Fax: +1-469-983-0095
