Understanding Medical Billing Charges
So what are the medical billing companies really charging and more to the point, what are you actually being charged?
On paper, it can be so easy. Here a percentage and there a flat fee. But in reality? It is not just a line charge on your medical billing, but an actual lever on your revenue, cash flow, and operational sanity.
The reason why most vendors will not tell you this, in detail, is because cheap billing is costly billing.
When claims are being denied, underpaid, or not pursued, the low percentage is meaningless. And a higher fee? It can easily offset itself when it generates income that you were losing before.
The question is not then how much does billing cost?
It is how much am I putting up on the table without the right billing partner?
This blog will dissect just how medical billing firms charge their services, what determines those charges and how to determine whether you are getting a pay back or it is another cost.

The Hidden Cost of Getting Medical Billing Wrong
Most practices understand that medical billing is complicated. What many do not fully appreciate is just how expensive that complication becomes when it is not managed well. The medical billing service cost paid to an outsourced partner is visible and easy to evaluate. On the other hand, the cost of poor billing performance is invisible hidden in the gap between what is billed and what is actually collected.
Consider what happens when claims are submitted with errors. They are denied. Resubmission takes time. Payers impose deadlines. Some claims age past the point of recovery. Meanwhile, the practice’s cash flow suffers, AR days climb, and the billing team, overwhelmed by rework, allows new errors to compound the problem.
Studies show that up to 30% of medical claims face challenges before they are paid. Practices handling billing in-house, without the right tools or expertise, see denial rates of 10% to 25% which is far above what is achievable with a high-performing outsourced billing partner. The medical billing costs per claim doubles rapidly when denial management is reactive rather than proactive.
What Do Medical Billing Services Really Cost?
Now that the problem and the solution have been established, a thorough understanding of medical billing pricing structures is worth building. Knowing how medical billing company fees are structured empowers practices to ask the right questions, compare vendors accurately, and recognize when a quoted rate represents genuine value versus a race to the bottom.
The three main medical billing pricing structures used across the industry are explained below. Each has its place and understanding the differences is essential to making a smart, informed decision for any practice.
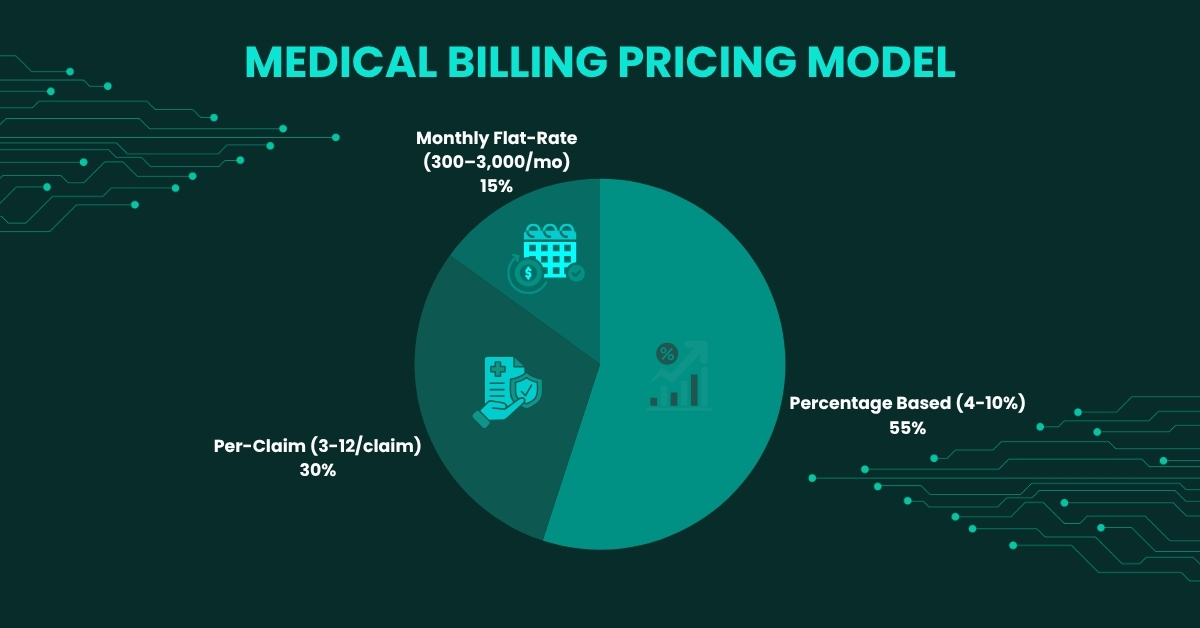
Medical Billing Rates by Specialty: Where Does Your Practice Fall?
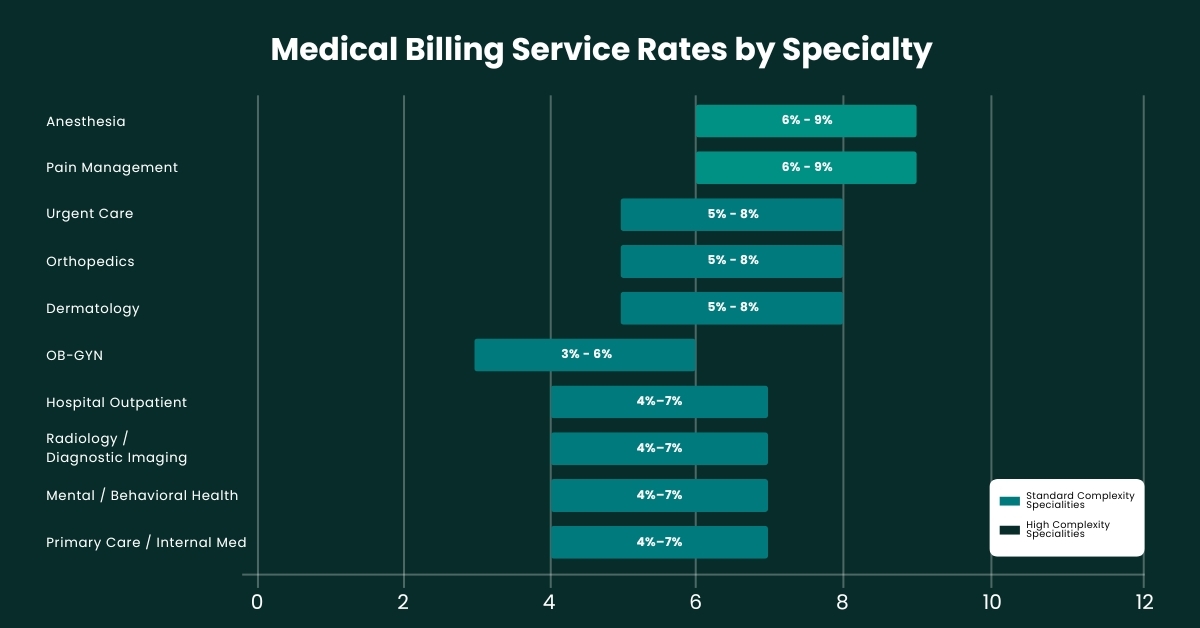
One of the most common points of confusion when evaluating medical billing company rates is the assumption that all specialties are priced the same. They are not — and they should not be. The coding complexity, denial risk, and payer negotiation demands of anesthesia billing are fundamentally different from those of primary care. Pricing that does not reflect these differences either overcharges simple practices or underserves complex ones.
At Vigilant Medical Group, pricing is specialty-specific. The chart and table below show how medical billing service rates vary across ten major specialties — and what drives those differences in real terms.
Medical Billing Rates by Practice Type
| Practice Type | Typical % of Collections | Estimated Monthly Cost | Common Pricing Model | Key Notes |
|---|---|---|---|---|
| Hospitals / Large Health Systems | 2% – 5% | $20,000 – $100,000+ | Custom enterprise contracts | Lower % due to very high claim volume and economies of scale |
| Solo Practices (1 Provider) | 5% – 10% (up to 12%) | $800 – $2,500+ | % of collections or per-claim | Higher % due to low volume and fixed operational costs |
| Group Practices (2–10 Providers) | 4% – 8% | $3,000 – $12,000 | % of collections | Most common pricing range; balanced volume and workload |
| Multi-Specialty Clinics | 3% – 6% | $12,000 – $45,000+ | Tiered % or hybrid | Lower % but higher total cost due to complexity and specialties |
| Urgent Care Centers | 5% – 9% | $5,000 – $20,000+ | % or per-claim | High patient turnover and volume increase billing workload |
| Telehealth / Virtual Practices | 4% – 8% | $1,000 – $10,000+ | % or per-claim | Lower overhead but payer variability affects billing complexity |
| Direct Primary Care (DPC) | 2% – 5% (if billing used) | Minimal / optional | Flat fee or minimal billing | Often subscription-based; limited insurance billing required |
1. Percentage-Based Charges: The Performance-Aligned Model
Under the percentage-based model, the billing company is paid a percentage of whatever collections are processed on the practice’s behalf. This is the most widely used medical billing pricing structure in the United States. When the billing company’s revenue is tied directly to the practice’s collections, both parties share the same goal: maximize reimbursements.
At Vigilant Medical Group, a percentage-based model is used precisely because of this alignment. The practice never pays more than it collects. At Vigilant, every claim is pursued with the same urgency a practice owner would apply if billing were being done personally.
Average medical billing percentage: 4% to 10% of collected revenue, depending on specialty, volume, and scope of services.
| Service Type | Typical % Range | Notes |
|---|---|---|
| Full-Service Medical Billing | 4% – 9% | Most common for physician practices |
| High-Complexity Specialties (Anesthesia, Pain Mgmt) | 6% – 10% | Higher due to coding complexity |
| Hospital / Facility Billing | 3% – 7% | Higher volume, often lower rate |
| Patient Billing Only | 2% – 6% | Limited scope services |
| Urgent Care / Walk-In Clinics | 5% – 8% | High volume, multi-payer environment |
As the table illustrates, Aetna’s commercial window of 90–120 days is broadly in line with commercial norms across the industry. The outlier to watch is Original Medicare, which provides 12 full calendar months under 42 CFR § 424.44,a timeline that does not apply to Medicare Advantage plans sold through Aetna or any other private insurer.
2. Per-Claim (Flat Fee) Pricing
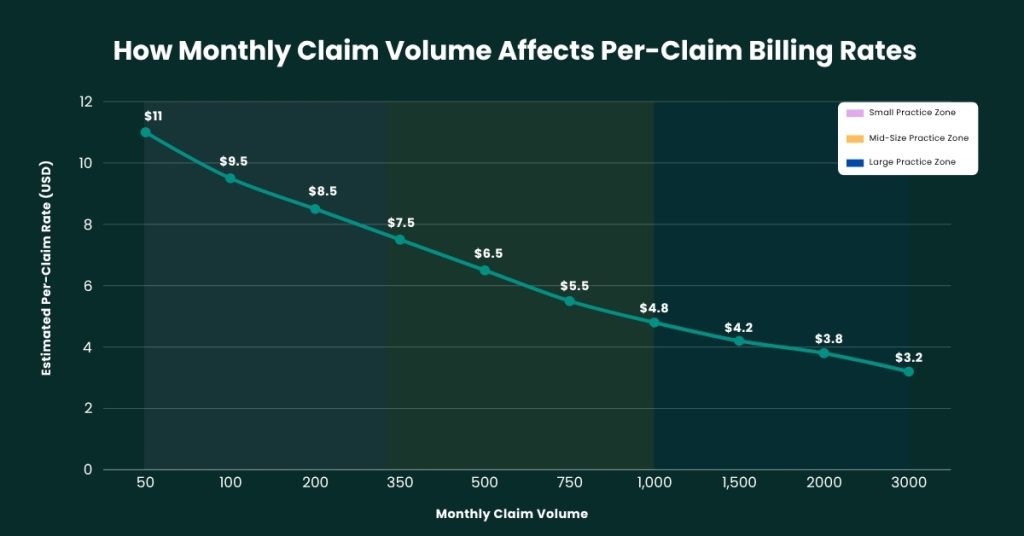
With the per-claim model, a fixed fee is charged per claim submitted regardless of the claim’s dollar value. This structure can seem appealing because it makes medical billing costs per claim easy to forecast month to month. However, it carries a risk: the billing company earns the same fee whether a claim is pursued aggressively or allowed to age without follow-up.
For practices with very high claim volumes and uniform claim values, per-claim pricing can offer savings. But for the majority of practices, particularly those in complex specialties, the percentage-based model delivers meaningfully better outcomes. The question of how much do medical billers charge per claim is answered below.
Medical billing rates per claim: $3.00 to $12.00 per claim, with variation by specialty, volume, and service scope.
| Practice Type | Est. Monthly Claims | Per-Claim Rate | Est. Monthly Cost |
|---|---|---|---|
| Small Solo Practice | 50 – 150 | $5 – $10 | $250 – $1,500 |
| Mid-Size Group Practice | 300 – 700 | $4 – $8 | $1,200 – $5,600 |
| Large Multi-Specialty Group | 700 – 2,000+ | $3 – $6 | $2,100 – $12,000 |
| Hospital Outpatient Dept. | 1,500 – 5,000+ | $2 – $5 | $3,000 – $25,000 |
3. Monthly Flat-Rate Pricing: Predictability at the Cost of Performance
Some billing companies offer a fixed monthly subscription fee covering a defined bundle of services. This model is favored by practices that want medical billing costs to be completely predictable regardless of revenue fluctuations. The concern with flat-rate pricing, however, is the same as with per-claim: because the billing company earns a fixed amount no matter how well claims perform, there is no built-in incentive to push for maximum reimbursement.
Typical flat-rate range: $300 to $3,000+ per month. Understanding how much billing companies charge under this model requires a careful, line-by-line scope review. Many services are excluded and priced separately.
The Fees Most Billing Companies Hope You Never Ask About
Medical billing company fees are rarely as simple as the headline rate suggests. For many billing companies, the base percentage or per-claim rate is just the beginning. A full picture of medical billing service fees must include setup costs, EHR integration charges, denial management add-ons, analytics subscriptions, and AR recovery commissions, each of which can significantly inflate the true medical billing service cost.
The table below compares the fees commonly found in the marketplace with how Vigilant Medical Group approaches each one. Transparency is not just a value at Vigilant, it is rather a competitive advantage.
| Fee Type | Typical Market Range | Vigilant Medical Group |
|---|---|---|
| Setup / Onboarding Fee | $200 – $1,500 | No hidden setup fees — ever |
| EHR Integration Fee | $100 – $500 | Included in onboarding at no charge |
| Credentialing Services | $75 – $200 per provider | Available with full transparency |
| Denial Management | Often 1% – 3% extra | Always included in core service |
| Reporting & Analytics Dashboard | $50 – $300/month | AI-powered BI Dashboard included free |
| Aged AR Recovery | 20% – 35% of recovered amount | Included in full-service plans |
| Patient Billing Statements | $0.50 – $2.00 per statement | Included as part of standard service |
Don’t Pay for Mediocre Billing Any Longer
Every month without a high-performing billing partner is revenue lost permanently. The Vigilant Medical Group can fix that. Start now.
There Is a Better Way and It Starts With Vigilant Medical Group
Vigilant Medical Group was built precisely for this problem. It is not a generic billing clearinghouse. It is a specialized, AI-enhanced revenue cycle management partner that has been trusted by healthcare providers across the United States to do one thing exceptionally well: ensure that every hard earned dollar through patient care is actually collected.
The difference between Vigilant Medical Group and the average billing company is not just in the medical billing service rates charged, it is in the outcomes delivered. Every claim is scrubbed before submission. Every denial is pursued. Every aging receivable is followed up. Every provider gets real-time visibility into their financial performance through an AI-powered Business Intelligence Dashboard, at no extra charge.
The result is not just cleaner billing. It is a fundamentally transformed revenue cycle that pays for the service fee many times over and then keeps paying.


The Real Cost of In-House Billing: A Number That Will Surprise Most Practices
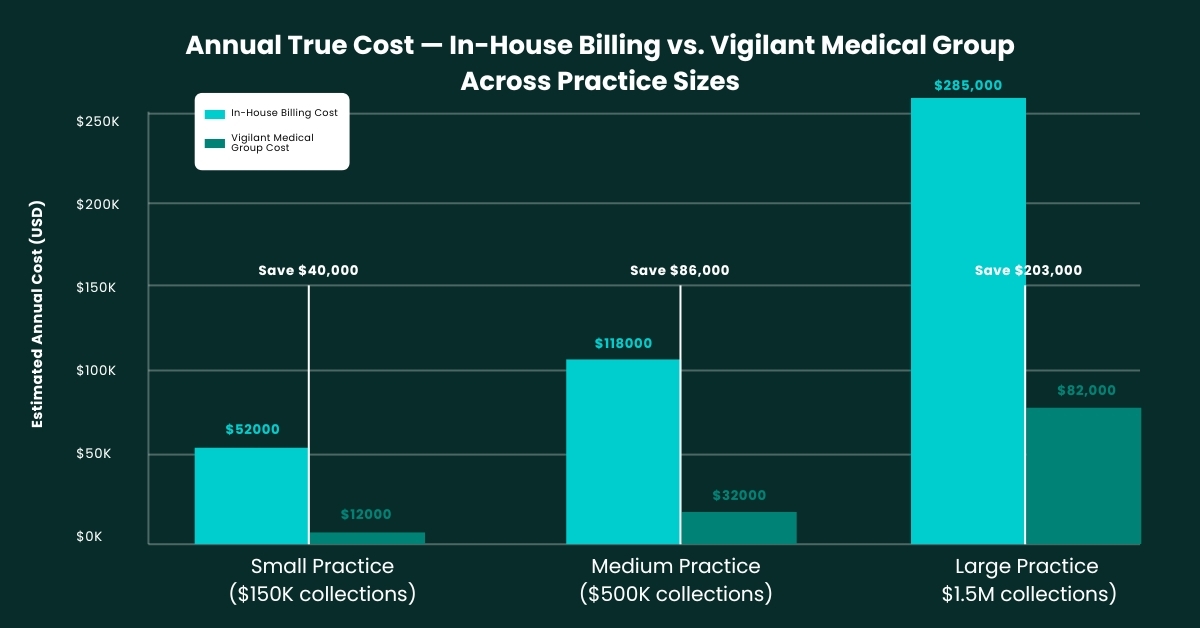
When the conversation turns to medical billing costs, practices often make the mistake of comparing outsourced billing fees against zero. The true comparison should always be against the fully-loaded, all-in cost of in-house billing a number that, when honestly calculated, almost always reveals outsourcing to be the smarter financial decision.
In-house billing carries a cost structure that is largely invisible because it is distributed across payroll, software, training, lost productivity, and the revenue that quietly disappears through denial rates that simply cannot match what a specialized, AI-powered partner achieves. The chart below makes that comparison concrete.
| Cost Category | In-House Billing (True Annual Cost) | Outsourced to Vigilant Medical Group |
|---|---|---|
| Billing Staff Salary (1 FTE) | $45,000 – $65,000 | Included in service |
| Payroll Taxes & Benefits (~30%) | $13,500 – $19,500 | None — zero overhead |
| Billing Software License | $1,200 – $15,600 | Fully included |
| Training & Continuing Education | $1,000 – $3,000 | None required |
| Turnover Risk & Recruitment | Variable — often severe | Zero exposure, guaranteed continuity |
| Average Denial Rate | 15% – 25% of claims | < 2% with Vigilant |
| First-Pass Claim Acceptance | Typically 70% – 85% | 98%+ guaranteed by Vigilant |
| Real-Time Analytics & Reporting | Rarely available in-house | AI BI Dashboard included — free |
| Effective Cost to Collect $1.00 | ~$0.137 (MGMA data) | ~$0.054 (industry outsourced average) |
The arithmetic is clear. A practice collecting $500,000 annually spends roughly $68,500 collecting in-house versus approximately $27,000 with Vigilant Medical Group before a single dollar of recovered denied claims is counted.
MGMA data shows in-house billing costs 13.7 cents per dollar collected. Outsourced billing averages 5.4 cents. For a $1 million practice, that gap represents over $82,000 in annual savings, before factoring in the revenue gained from Vigilant’s 98%+ first-pass acceptance rate.
Outsourcing to Vigilant vs. In-House Billing
| ✅ PROS (Outsource to Vigilant) | ❌ CONS (Keep Billing In-House) |
|---|---|
| 98%+ first-pass claim acceptance — fewer rejections, faster cash | Monthly service fee is a real though justified expense |
| AI-powered scrubbing catches every error before submission | Onboarding and initial data migration require time investment |
| Real-time BI Dashboard included, full financial visibility always | Less direct daily oversight of individual billing staff |
| Certified coders for every major specialty, no generalists | Some dependency on billing partner's communication quality |
| HIPAA-compliant, fully encrypted billing workflows throughout | Brief transition period may slow workflow initially |
| Zero hiring, training, or HR overhead | In-house billing expertise gradually diminishes over time |
| Faster reimbursements and meaningfully shorter AR cycles | Existing billing staff may resist or resent the change |
| Fully scalable as the practice grows | Poor-quality billing vendors do exist |
| Denial management and appeals included — nothing slips through | Contract terms vary; lock-in periods exist at some companies |
| 24/7 AI-powered revenue cycle oversight and monitoring | Requires a communication rhythm to stay aligned with partner |
| Credentialing and enrollment handled alongside billing | Some practices feel loss of direct control in early months |
| Transparent pricing | Ambiguity exists |
What Vigilant Medical Group Actually Charges and What That Fee Includes
Here is the part most billing companies deflect with vague language. Vigilant Medical Group operates on a performance-aligned, percentage-based medical billing pricing model because it is the model most aligned with the practice’s success. The Vigilant team earns more only when the practice collects more. That alignment is not incidental. It is by design.
Every Vigilant engagement begins with a free billing audit and a fully customized pricing proposal. There is no guesswork, no hidden medical billing company fees that surface after the contract is signed, and no bloated add-ons for services that should be standard. The table below reflects indicative ranges, actual pricing is determined through a detailed discovery conversation with every prospective client.
| Practice Type | Typical Rate Range | What Is Included |
|---|---|---|
| Solo Physician Practice | 5% – 8% of collections | Full RCM + coding + AR + denial management + AI dashboard |
| Small Group Practice (2–5 providers) | 4% – 7% of collections | Full RCM + credentialing + real-time reporting |
| Multi-Specialty Group | 4% – 6% of collections | Full RCM + BI Dashboard + EHR integration |
| Hospital / Facility Billing | 3% – 6% of collections | Full revenue cycle + compliance reporting |
| Anesthesia / Pain Management | 6% – 9% of collections | Specialty coding + time capture + denial defense |
| Urgent Care / Walk-In | 5% – 8% of collections | High-volume billing + real-time eligibility checks |

Everything Included in Vigilant Medical Group's Core Service
When practices evaluate medical billing services fees, the services menu is often where the real value gap between providers is revealed. A low percentage rate is meaningless if denial management costs extra, if reporting is locked behind a premium tier, or if credentialing is handled by a separate vendor at separate cost. At Vigilant Medical Group, none of that is the case.
Every item below is included as standard in a Vigilant Medical Group engagement — not as an upsell, not as a premium tier, and not subject to a separate billing company fee:
- Eligibility Verification: Real-time insurance verification before every patient encounter, blocking downstream denials before they can occur.
- Specialty-Specific Coding: ICD-10, CPT, and HCPCS coding performed by certified coders trained in the client’s specialty, not generic billers applying cookie-cutter codes.
- AI-Powered Claim Scrubbing: Every single claim is reviewed by AI and experienced billers before submission, sustaining Vigilant’s 98%+ clean claim rate.
- Electronic Claim Submission: Fast, accurate submission to all major commercial payers, Medicare, Medicaid, and managed care plans.
- Payment Posting & Reconciliation: Accurate matching of payments from EOBs, ERAs, virtual credit cards, checks, and bank deposits.
- Denial Management & Appeals: Proactive denial pattern analysis, error correction, and timely, aggressive appeal filing all included.
- Accounts Receivable Follow-Up: Persistent, systematic follow-up on every unpaid and aging claim until resolution, minimizing revenue leakage.
- Patient Billing & Statements: Clear, accurate, patient-friendly statements that reduce confusion and support faster patient payment.
- Credentialing & Enrollment: Provider credentialing and payer enrollment to prevent billing delays and maintain compliance with payer requirements.
- AI Business Intelligence Dashboard: Real-time visibility into claims, collections, aging, and performance, available 24/7, always included at no charge.
- HIPAA Compliance & Data Security: Every workflow operates under strict HIPAA protocols with encrypted systems protecting all patient and practice data.
Vigilant’s AI-powered Business Intelligence Dashboard (BID) classifies every claim into four clear categories. In Process, Fully Paid, Partially Paid, or Denied, giving practice owners and managers complete financial clarity at any moment, without chasing their billing team for updates.
Every Day Without the Right Billing Partner Is Revenue Lost for Good
Medical billing is not an administrative function that can be left to chance, deferred to an overburdened in-house team, or entrusted to a generic billing vendor. It is the financial engine of every healthcare practice and when that engine underperforms, the consequences accumulate silently and permanently.
The question of what medical billing companies charge has now been answered in full. The more important question, the one that will determine the financial health of a practice for years to come is which medical billing partner will actually deliver what it promises.
Vigilant Medical Group has built its reputation on one answer to that question. A 98%+ first-pass claim acceptance rate, a denial rate below 2%, AI-powered revenue intelligence, certified specialty coders, and a team that pursues every dollar with the same commitment as the physician who earned it. That is not a promise made on a website. It is a performance record built one claim at a time.
The free billing audit is available right now. It will show exactly what is being left on the table and exactly what Vigilant Medical Group will do to recover it.
- Join hundreds of healthcare providers nationwide who have already transformed their billing with Vigilant Medical Group.
- ✅ Free Billing Audit | ✅ Custom Pricing Proposal | ✅ No Obligation




